Ischemic stroke
The gold standard in stroke care
Trusted by leading healthcare providers worldwide, our ischemic stroke solutions deliver unmatched clinical depth. Used in patient selection for the landmark trials that shaped the AHA’s updated guidelines, RapidAI is redefining what’s possible in stroke diagnosis and treatment.

Lumina 3D™ by RapidAI
Access advanced 3D imaging reconstruction minutes after a head and neck CTA scan
-
Consistent, high quality reconstructions 24/7: Detailed 3D views expedite diagnosis across a range of neurovascular cases
-
Roadmap on the go: Visualize the aortic arch, carotid tortuosity, and distal neurovasculature from your mobile device
-
Fully automated: Increase CT scanner throughput and maximize radiology tech resources, saving significant hours per month
Your complete ischemic stroke solution
NCCT Stroke
ASPECTS
Hypodensity
Rapid LMVO
Rapid CTA
Perfusion Imaging
AngioFlow

NCCT Product
Rapid NCCT Stroke
Improve equity of care with the only FDA-cleared NCCT imaging solution for suspected LVO
-
Make early and time-sensitive treatment and transfer decisions
-
Enable stroke detection at any center, for equitable care across the network
-
Expedite time between CT and CTA scans with prompt LVO notifications
image analysis
increase in sensitivity
faster with Rapid vs no Rapid in time-to-decision
NCCT Product
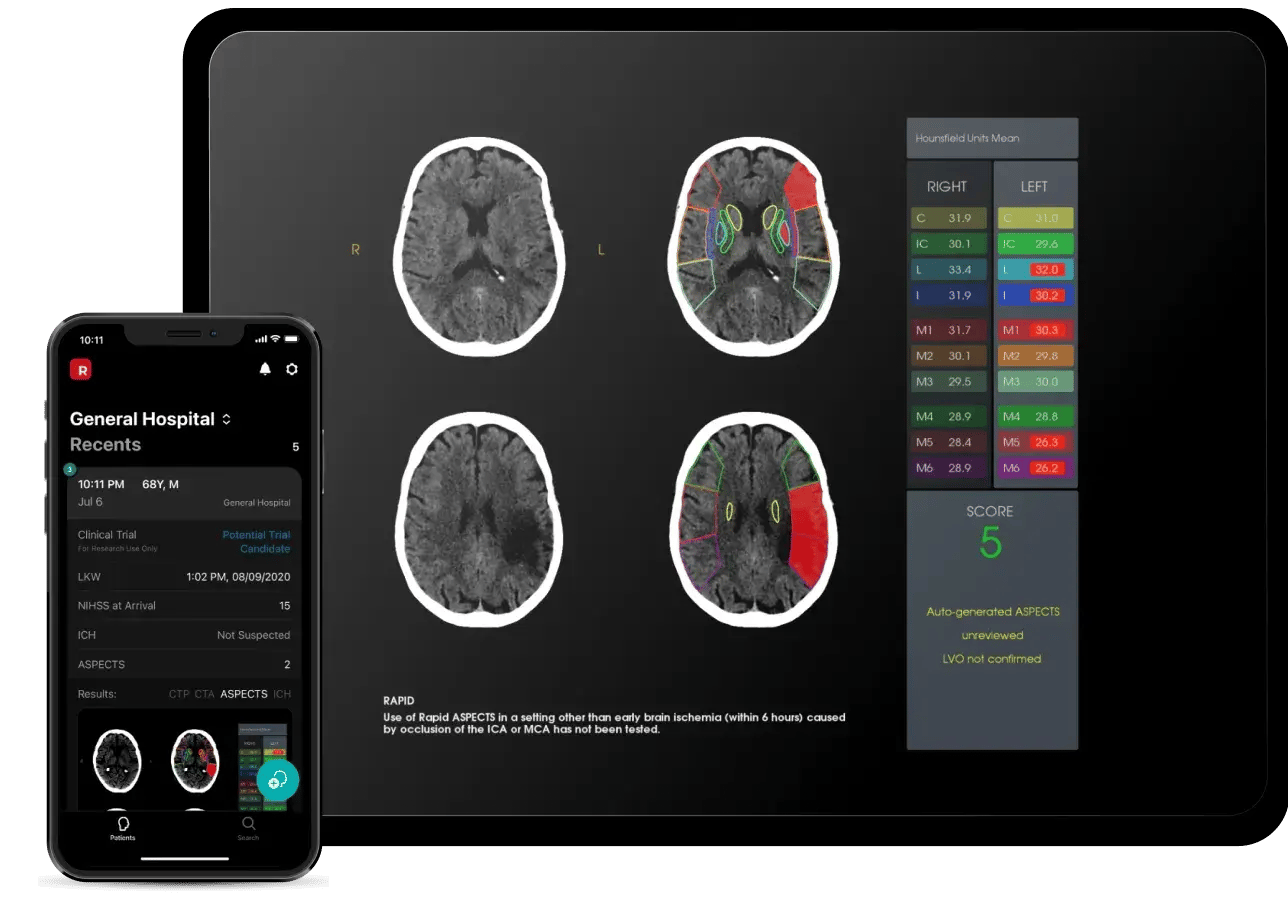
Rapid ASPECTS
The first neuro-imaging AI solution shown to improve clinician diagnostic accuracy
-
Determine thrombectomy eligibility with an automated ASPECT score
-
Quickly visualize regions of asymmetry and review measurements of ischemic change
-
Help every reader be an expert – increase reader reliability and reduce intra-reader variability
< 2 minutes - standardized ASPECT score delivered
improvement in reader accuracy
NCCT Product
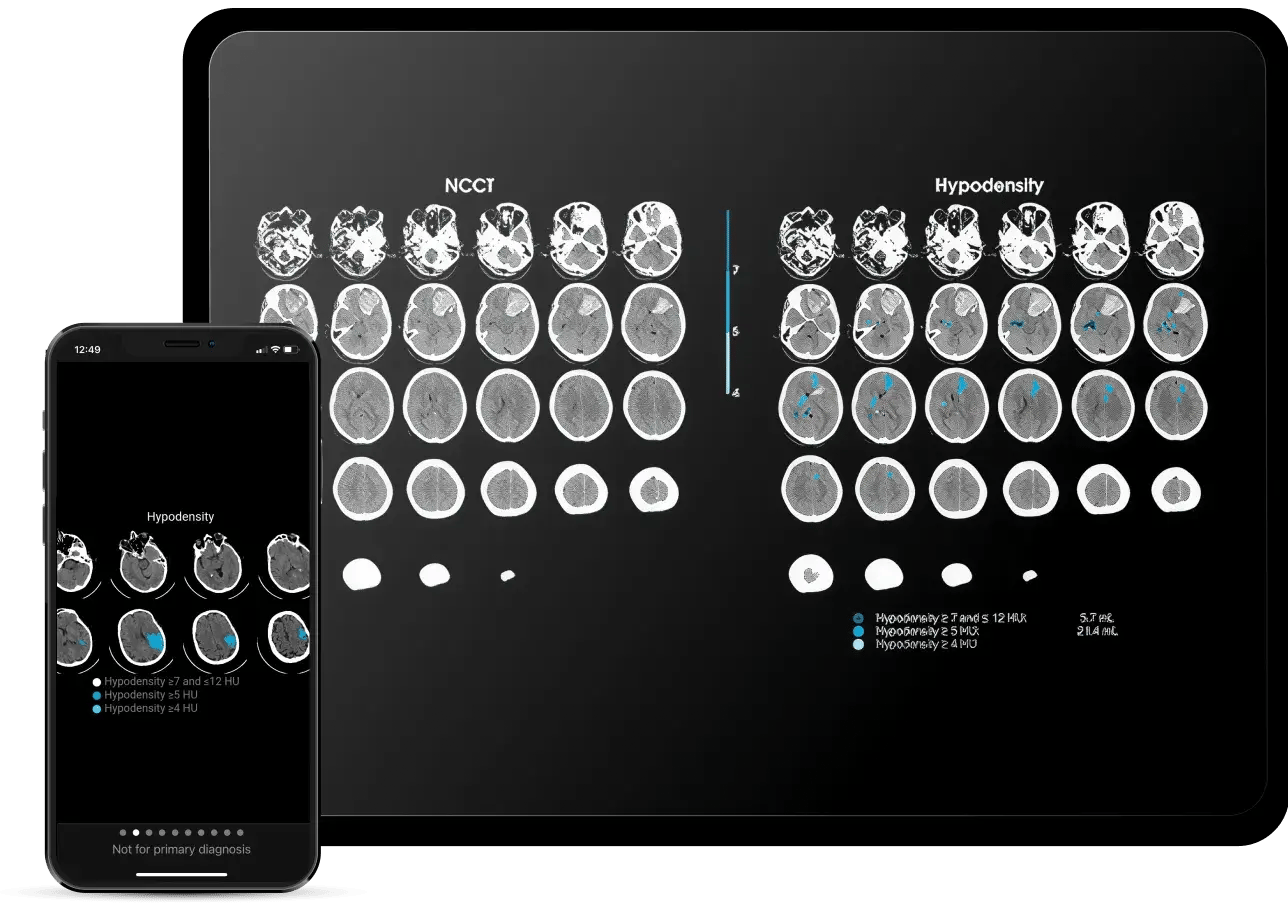
Rapid Hypodensity
The first software to help identify and quantify potential subacute infarction volumes across all brain regions
-
Easily visualize the extent and region of ischemia, differentiating between subacute and chronic lesions
-
Determine the best treatment decisions for large core patients
-
Get NCCT results in minutes, including regions with HU reductions between 4-12
First and only solution to provide automated quantification of hypodense tissue after an ischemic event

CTA Product
Rapid LMVO
Complete brain occlusion triage with complete confidence
-
Detect suspected vessel occlusions in the ICA, MCA, ACA, Basilar and PCA
-
27% more patients triaged when compared to Rapid LVO2
-
Introducing AI Education overlay for transparency into AI findings
CTA Product
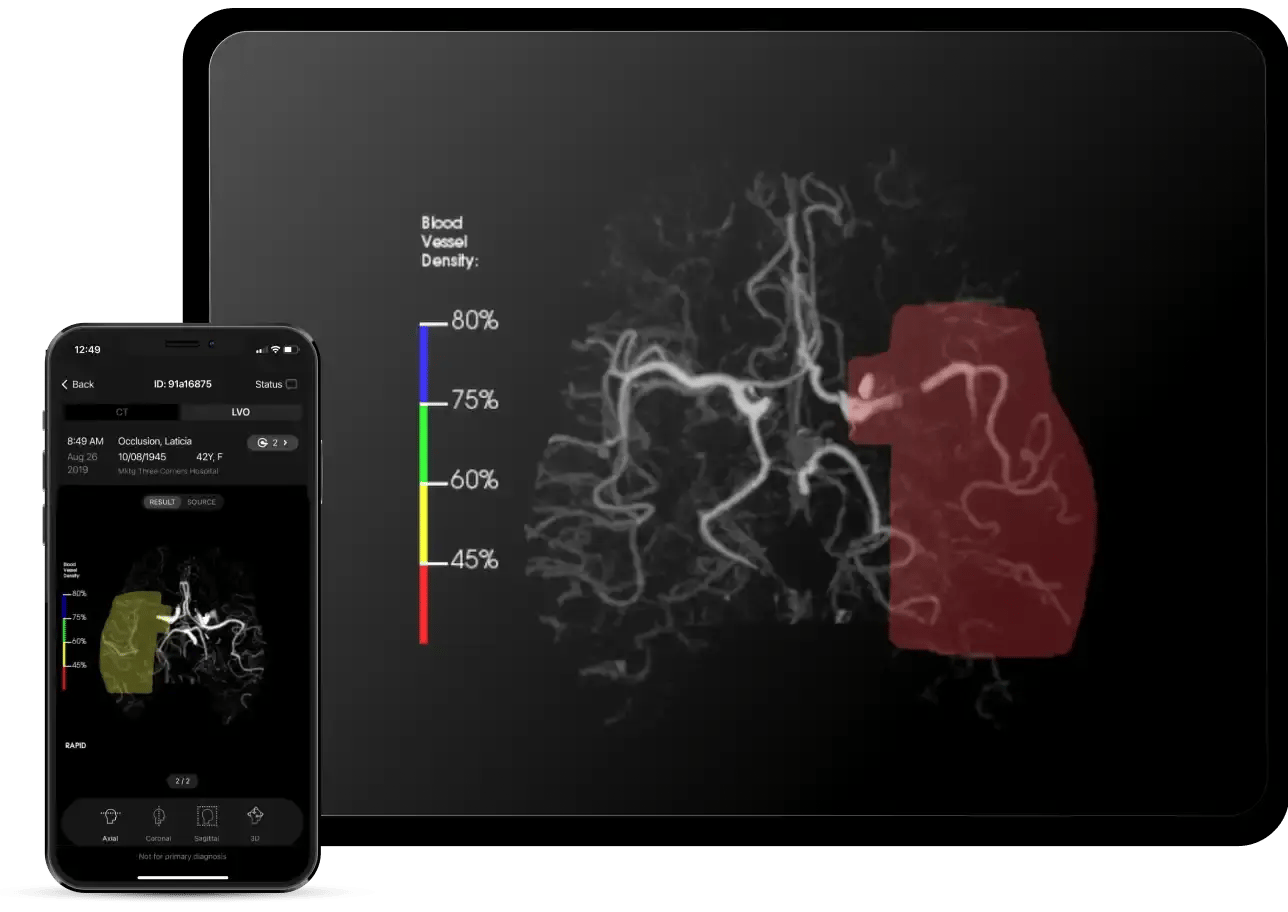
Rapid CTA
Enhance your visibility of distal occlusions and collateral flow with vessel density asymmetry
-
Identify the area of occlusion and quantify the impacted vasculature with color-coded overlays
-
Automatically assess collateral vessels to inform treatment and prognostic decisions
-
Enhance your view with 3D reconstructions and multi-angle perspectives for precise stroke diagnosis
MeVOs Identified with Rapid Ischemic Stroke Solution (Rapid LVO + Rapid CTA Vessel Density)3
PPV for LVOs4
reduction in CTA-to-Groin puncture5
CTP Product
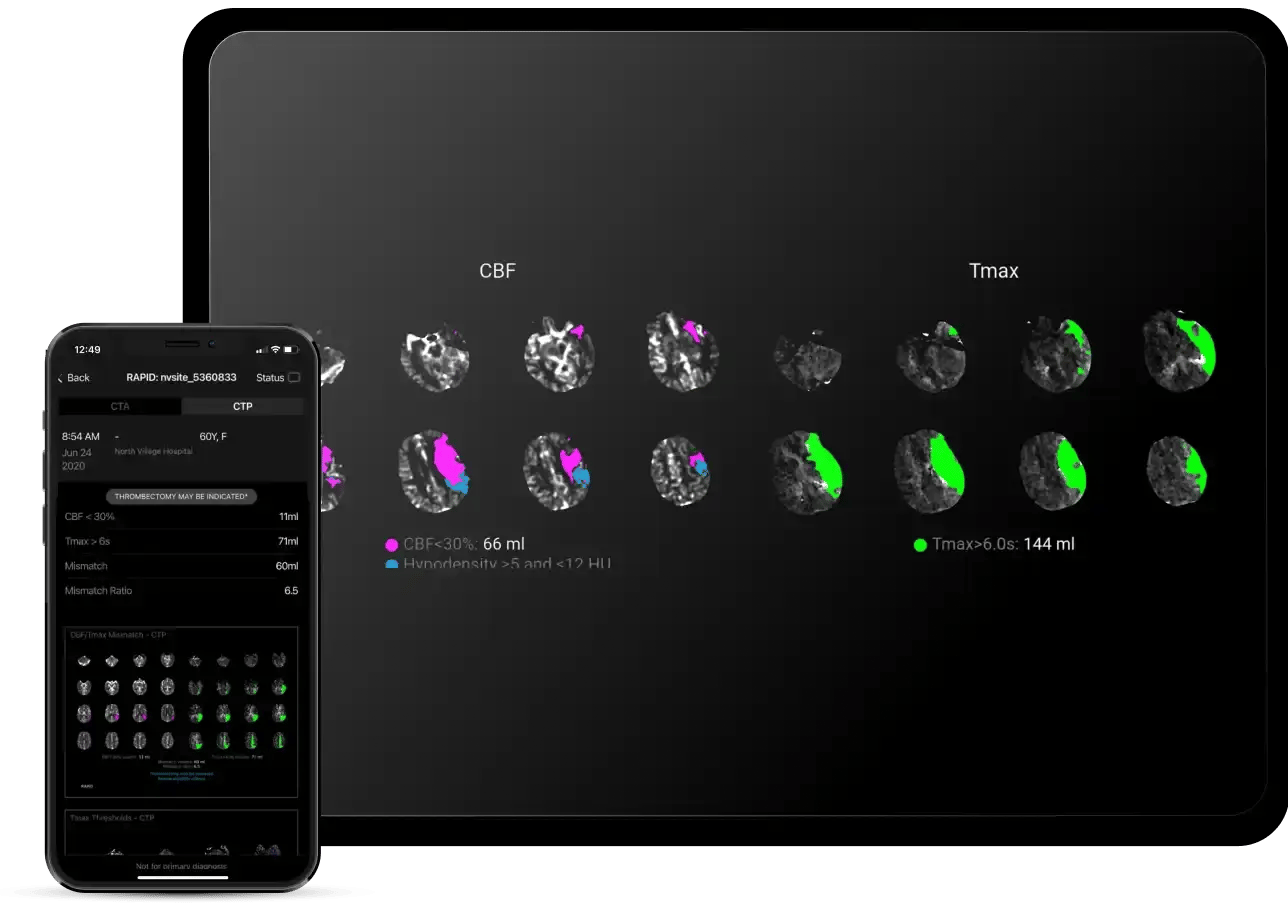
Rapid Perfusion Imaging
The only perfusion imaging solution cleared in the U.S. with a mechanical thrombectomy indication
-
Identify salvageable brain tissue with quantified, color-coded maps of ischemic core and penumbra mismatch
-
Project ischemic core growth and collateral capability with hypoperfusion
-
Consolidate a wide range of complex data into easily visualized outputs of cerebral blood flow (CBF), cerebral blood volume (CBV), transit times (MTT and Tmax) with integrated scan quality controls
-
Rapid CTP has been the core technology at the center of many of the pivotal stroke trials and continues to be the gold standard in 75% of all Comprehensive Stroke Centers in the US
>10 Clinical trials. Validate Rapid CTP, including EXTEND, SWIFT-PRIME, DAWN, EXTEND-IA, AND DEFUSE 3.
increase in Mechanical Thrombectomy procedures post RapidAI implementation6
90/95% Sen/Spec for distal vessel occlusion7
CTP Product
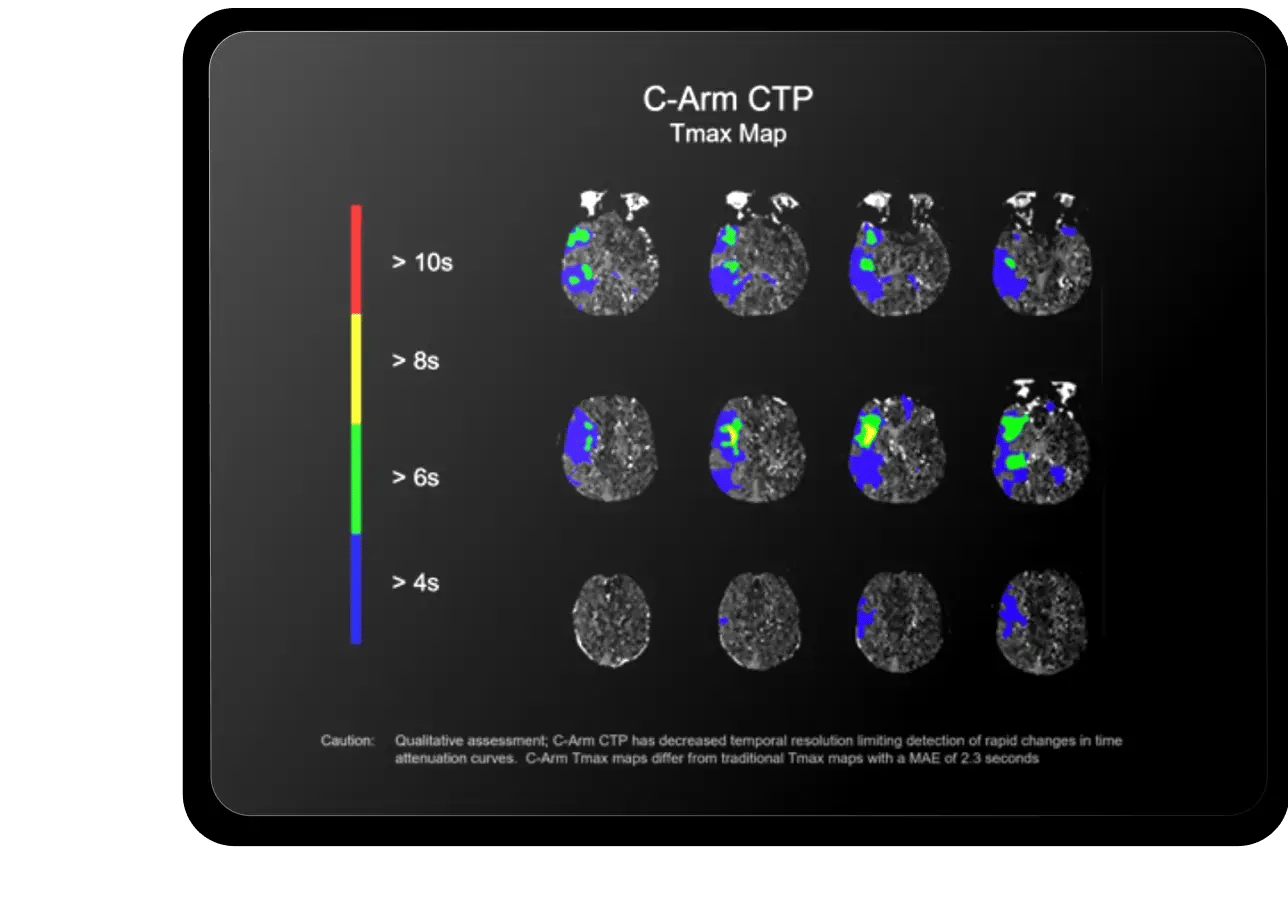
AngioFlow by RapidAITM
Accelerate time to treatment with perfusion imaging in the angio suite
-
Take the patient directly to the angio suite and review qualitative assessments
-
Reduce the need for re-imaging ahead of surgery to save time and resources while improving workflow
-
Review color-coded brain regions with reduced CBF/CBV and delayed contrast arrival in the angio suite
-
Identify irreversibly injured tissue and assess successful reperfusion directly on the C-Arm
time saved with direct-to-angio LVO patient routing8
mRS improvement9
NCCT Stroke
ASPECTS
Hypodensity
LMVO
CTA
Perfusion Imaging
AngioFlow
Lumina

NCCT Stroke
Improve equity of care with the only FDA-cleared NCCT imaging solution for suspected LVO
-
Make early and time-sensitive treatment and transfer decisions
-
Enable stroke detection at any center, for equitable care across the network
-
Expedite time between CT and CTA scans with prompt LVO notifications
image analysis
increase in sensitivity
faster with Rapid vs no Rapid in time-to-decision

Rapid ASPECTS
The first neuro-imaging AI solution shown to improve clinician diagnostic accuracy
-
Determine thrombectomy eligibility with an automated ASPECT score
-
Quickly visualize regions of asymmetry and review measurements of ischemic change
-
Help every reader be an expert – increase reader reliability and reduce intra-reader variability
standardized ASPECT score delivered
improvement in reader accuracy

Rapid Hypodensity
The first software to help identify and quantify potential subacute infarction volumes across all brain regions
-
Easily visualize the extent and region of ischemia, differentiating between subacute and chronic lesions
-
Determine the best treatment decisions for large core patients
-
Get NCCT results in minutes, including regions with HU reductions between 4-12
solution to provide automated quantification of hypodense tissue after an ischemic event

Rapid LMVO
Complete brain occlusion triage with complete confidence
-
Detect suspected vessel occlusions in the ICA, MCA, ACA, Basilar and PCA
-
27% more patients triaged when compared to Rapid LVO(2)
-
Introducing AI Education overlay for transparency into AI findings

Rapid CTA
Enhance your visibility of distal occlusions and collateral flow with vessel density asymmetry
-
Identify the area of occlusion and quantify the impacted vasculature with color-coded overlays
-
Automatically assess collateral vessels to inform treatment and prognostic decisions
-
Enhance your view with 3D reconstructions and multi-angle perspectives for precise stroke diagnosis
MeVOs Identified with Rapid Ischemic Stroke Solution (Rapid LVO + Rapid CTA Vessel Density)3
PPV for LVOs4
reduction in CTA-to-groin puncture5

Rapid Perfusion Imaging
The only perfusion imaging solution cleared in the U.S. with a mechanical thrombectomy indication
-
Identify salvageable brain tissue with quantified, color-coded maps of ischemic core and penumbra mismatch
-
Project ischemic core growth and collateral capability with hypoperfusion
-
Consolidate a wide range of complex data into easily visualized outputs of cerebral blood flow (CBF), cerebral blood volume (CBV), transit times (MTT and Tmax) with integrated scan quality controls
-
Rapid CTP has been the core technology at the center of many of the pivotal stroke trials and continues to be the gold standard in 75% of all Comprehensive Stroke Centers in the US
Clinical trials validate Rapid CTP, including EXTEND, SWIFT-PRIME, DAWN, EXTEND-IA, AND DEFUSE 3
increase in Mechanical Thrombectomy procedures post RapidAI implementation6
Sen/Spec for distal vessel occlusion7

AngioFlow by RapidAITM
Accelerate time to treatment with perfusion imaging in the angio suite
-
Take the patient directly to the angio suite and review qualitative assessments
-
Reduce the need for re-imaging ahead of surgery to save time and resources while improving workflow
-
Review color-coded brain regions with reduced CBF/CBV and delayed contrast arrival in the angio suite
-
Identify irreversibly injured tissue and assess successful reperfusion directly on the C-Arm
time saved with direct-to-angio LVO patient routing8
mRS improvement9

Lumina by RapidAI™
- Consistent, high quality reconstructions 24/7: Detailed 3D views expedite diagnosis across a range of neurovascular cases.
- Roadmap on the go: Visualize the aortic arch, carotid tortuosity, and distal neurovasculature from your mobile device
- Fully automated: Proven to save thousands of radiology tech hours per month and increase CT scanner throughput
Improving outcomes for patients and populations
Hear real-world perspective on how RapidAI helps transform individual care and drive system-wide impact.
How it works: fast, connected, and ready for action
From scan to intervention, RapidAI keeps the entire team
informed + connected.
-
Scan initiated: After a scan, our deep clinical AI automatically processes the images within moments
-
Prompt results: Results are instantly delivered to the care team—accessible through the mobile app, PACS, and integrated systems
-
Real-time collaboration: Teams can discuss findings and next steps directly within the platform
-
Coordinated action: When intervention is needed, the team can be quickly activated to deliver care

Clinical Solutions
Expand the reach of your expertise
Your “wow” moment
is a click away
Sources:
1. From a simulated study - Improved Time to Triage decision by emergency physicians using RAPID noncontrast CT stroke platform for acute stroke patients
2. Data on file. 1500 consecutive patient dataset comparing Rapid LVO and Rapid LMVO
3. (Sowlat, Mohammad Mahdi, et al. "Abstract WMP66: Detecting Medium Vessel Occlusions and Collateral Assessment With Multimodality AI Approach." Stroke 55.Suppl_1 (2024): AWMP66-AWMP66.)
4. (Amukotuwa, Shalini A et al. “Fast Automatic Detection of Large Vessel Occlusions on CT Angiography.” Stroke vol. 50,12 (2019): 3431-3438. doi:10.1161/STROKEAHA.119.027076
5. (Amukotuwa, Shalini A et al. “Fast Automatic Detection of Large Vessel Occlusions on CT Angiography.” Stroke vol. 50,12 (2019): 3431-3438. doi:10.1161/STROKEAHA.119.027076)
6. (Malisch, Tim W., et al. "Abstract WP126: Improved Stroke Outcomes Following Implementation of RapidAI Platform at Ascension-Illinois." Stroke 55.Suppl_1 (2024): AWP126-AWP126.)
7. (Amukotuwa, S A et al. “Time-to-Maximum of the Tissue Residue Function Improves Diagnostic Performance for Detecting Distal Vessel Occlusions on CT Angiography.” AJNR. American journal of neuroradiology vol. 42,1 (2021): 65-72. doi:10.3174/ajnr.A6891)
8. Desai, Shashvat M., et al. "Direct transfer to the neuroangiography suite for patients with stroke." Stroke 54.6 (2023): 1674-1684.
9. Galecio-Castillo, Milagros, et al. "Direct to angiosuite strategy versus standard workflow triage for endovascular therapy: systematic review and meta-analysis." Journal of neurointerventional surgery 15.e1 (2023): e17-e25.