Endovascular thrombectomy (EVT) has revolutionized stroke management.
DAWN and DEFUSE-3 trials and the AURORA meta-analysis provided evidence for EVT as the treatment option in selected ischemic stroke patients for up to 24 hours of last known well. Advanced imaging helped with patient selection.
What are the outcomes of treating patients with EVT beyond 24 hours of last known well?
Dr. Amrou Sarraj and co-authors performed a retrospective, multinational, multicenter cohort study and found EVT led to better functional independence in patients presenting beyond 24 hours of last known well. However, the EVT group had increased odds of symptomatic intracranial hemorrhage (sICH) compared with the medical management group (control).
Key takeaways:
- The EVT group achieved higher odds of functional independence than the control group (EVT, 38% vs. control, 10%; P < 0.001; inverse probability treatment weighting [IPTW] adjusted odds ratio [aOR], 4.56).
- However, the EVT group had significantly higher odds of sICH than the control group (EVT, 10.1% vs. control, 1.8%; P = 0.003; IPTW aOR, 10.65).
Study design
The patients included were:
- Adults (age ≥18 years)
- Diagnosed with large-vessel occlusion in the internal carotid artery or M1 or M2 segments of the middle cerebral artery
- Received treatment beyond 24 hours of stroke onset
- Patients from 17 high-volume EVT centers across the United States, Europe, and Australia between July 2012 and December 2021
Patients were divided into two groups based on the treatment received: EVT or medical management only (control). Physicians determined EVT eligibility on a case-by-case basis.
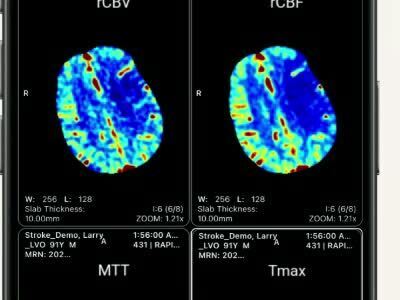
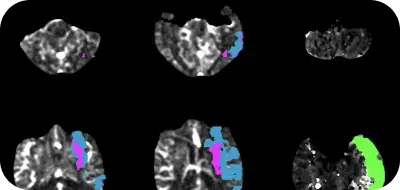
The Alberta Stroke Program Early CT Score(s) (ASPECTS) were evaluated on baseline non-contrast CT (NCCT) scans. The perfusion images were processed using Rapid CTP.
301 patients were included in this study, of which 185 received EVT and 116 received medical management.
Patient characteristics
When comparing EVT and control groups, they found the following:
- The EVT and control groups had similar median ages (EVT, 69 years vs. control, 68.5 years; P = 0.95)
- The EVT and control groups had a similar proportion of female patients (EVT, 86 of 181 [48%] vs. control, 63 of 115 [55%]; P = 0.22)
- The EVT and control groups had a similar proportion of patients with wake-up stroke (EVT, 31 of 153 [20%], vs. control, 22 of 111 [20%]; P = 0.93)
- The patients who received EVT demonstrated lower baseline stroke severity (median NIHSS score in EVT group, 14, vs. control, 17; P = 0.01)
- The patients who received EVT arrived earlier at an EVT-capable center (median time in EVT group, 28.1, vs. control, 31.4 hours; P = 0.002).
Imaging characteristics
The ischemic injury estimates were smaller in the EVT group on NCCT and CT perfusion (CTP).
- NCCT - median CT ASPECTS for EVT group, 7, vs. control group, 5; P < 0.001
- CTP - median ischemic core volume for EVT group, 4 mL, vs. control group, 13.4 mL; P = 0.004.
The critically hypoperfused tissue volumes (Tmax > 6) were similar in both groups - median volume, EVT group, 79 mL, vs. control group, 91 mL; P = 0.43.
Functional and safety outcomes
- EVT group achieved higher odds of functional independence (38% vs. control, 10%; P < 0.001; IPTW aOR, 4.56)
- EVT group had lower odds of mortality (26% vs. control, 41%; P = 0.02; IPTW aOR, 0.49).
- EVT group had significantly higher odds of sICH (10.1% vs. control, 1.8%; P = 0.003; IPTW aOR, 10.65).
The EVT group demonstrated better functional outcomes even when the patients were propensity-matched based on clinical and imaging characteristics (including mismatch ratio and volume) and analyzed.
This study is the largest to date evaluating EVT's functional and safety outcomes in ischemic stroke patients presenting beyond 24 hours of last known well compared to patients who received medical management only. Future prospective studies will help confirm these findings and evaluate the outcomes of EVT for patients beyond 24 hours last known well.
The RapidAI Clinical Affairs team works closely with physicians and healthcare systems worldwide to advance stroke care. Learn more about how we support clinical trials here.
Co-authors in this paper: Timothy J. Kleinig, MBBS(Hons), PhD; Ameer E. Hassan, DO; Pere Cardona Portela, MD; Santiago Ortega-Gutierrez, MD; Michael G. Abraham, MD; Nathan W. Manning, MD; James E. Siegler, MD; Nitin Goyal, MD; Laith Maali, MD; Spiros Blackburn, MD; Teddy Y. Wu, MBChB; Jordi Blasco, MD; Arturu Renú, MD; Navdeep S. Sangha, MD; Juan F. Arenillas, MD; Margy E. McCullough-Hicks, MD; Adam Wallace, MD; Daniel Gibson, MD; Deep K. Pujara, MBBS; Faris Shaker, MBChB; Mercedes de Lera Alfonso, MD; Marta Olivé-Gadea, MD; Mudassir Farooqui, MD; Juan S. Vivanco Suarez, MD; Zachary Iezzi, BS; Jane Khalife, MD; Colleen G. Lechtenberg, MD; Syed K. Qadri, MD; Rami B. Moussa, BS; Mohammad A. Abdulrazzak, MD; Tareq S. Almaghrabi, MBBS; Osman Mir, MD; James Beharry, MBChB; Balaji Krishnaiah, MD; Megan Miller, BS; Najwa Khalil, MBBS; Gagan J. Sharma, MS; Aristeidis H. Katsanos, MD; Ali Fadhil, MD; Kelsey R. Duncan, MD; Yin Hu, MD; Sheryl B. Martin-Schild, MD; Georgios K. Tsivgoulis, MD; Dennis Cordato, MBBS; Anthony Furlan, MD; Leonid Churilov, PhD; Peter J. Mitchell, MD; Adam S. Arthur, MD; Mark W. Parsons, MD; James C. Grotta, MD; Clark W. Sitton, MD; Marc Ribo, MD; Gregory W. Albers, MD; Bruce C. V. Campbell, MBBS, PhD