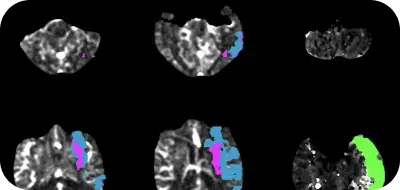
Pivotal trials helped establish the role of endovascular thrombectomy (EVT) treatment for selected ischemic stroke patients with large vessel occlusions. However, not all patients undergoing EVT receive functional independence.
What mediates clinical benefits in patients who have successful reperfusion? Is it a reduction in infarct growth, edema, or both?
Dr. Amrou Sarraj and co-authors quantified these mediators and studied their interrelationships.
Key takeaways:
- Reduced infarct growth and cerebral edema mediated ~80% of the successful reperfusion effect on functional outcomes.
- Future studies on other mediators of successful reperfusion effect can reveal new therapeutic targets to help enhance reperfusion benefits.
Study design
It was a pooled, patient-level post hoc analysis of patients from three randomized controlled trials (EXTEND IA, EXTEND IA TNK18 and EXTEND IA TNK) and one prospective study, SELECT.
The patients met the following inclusion criteria:
- Age >18 years old at the time of presentation
- Acute ischemic stroke caused by anterior circulation large vessel occlusion (ICA/M1 or M2 segment of MCA)
- Presented at an EVT capable center within 24 hours of last known well
- Available perfusion imaging parameters for analysis
- Angiogram-based evaluation of reperfusion grade
- Follow-up imaging to evaluate the volume of infarcted tissue
Patients who exhibited significant ischemic core overestimation were excluded from the analysis.
All CT and MR images were processed by Rapid software.
- The ischemic core was measured by calculating tissue volume with relative cerebral blood flow (rCBF) <30%.
- Critically hypoperfused tissue volume was defined using Tmax >6 sec.
- Successful reperfusion was defined as a modified treatment in cerebral ischemia score ≥2b (>50% reperfusion).
- Infarct volumes were measured using manual delineation of infarcted tissue on follow-up imaging.
- Infarct growth was defined as the volumetric difference between the ischemic core on baseline perfusion imaging and infarct volume on follow-up imaging.
- Cerebral edema was defined as a midline shift of at least 1mm on axial scan on follow/up CT/MR imaging.
The imaging evaluation to determine midline shift and infarct volume occurred between 24 hours and 7 days of successful reperfusion.
665 patients met the eligibility criteria. Of these patients, 542 (81.5%) achieved successful reperfusion, and 123 (18.5%) had unsuccessful reperfusion.
Patient characteristics
Patients in both unsuccessful and successful reperfusion groups had similar baseline clinical and imaging characteristics.
- Age (70.5 vs. 72 years, p=0.57)
- NIHSS (16 vs. 16, p=0.37)
- CT ASPECTS (9 vs. 9, p=0.94)
- Ischemic core (8.0 vs. 6.0 ml, p=0.35)
- Critically hypoperfused tissue volumes (122.0 vs. 116.9 ml, p=0.73).
However, successful reperfusion was associated with higher odds of functional independence (Adjusted odds ratio [aOR]=2.09, p=0.001) and better mRS scores (p<0.001).
Mediation of Successful Reperfusion Effect on Functional Independence by Infarct Growth and Midline Shift (or cerebral edema)
Successful reperfusion was independently associated with better mRS scores (P < 0.001) and reductions in infarct growth (P<0.001) and midline shift (P<0.001). However, the association between successful reperfusion and the improved functional outcome became insignificant (p=0.094) after adding infarct growth and midline shift to the model.
Infarct growth and midline shift explained 45% and 34% of the association between successful reperfusion and functional outcomes.
The decrease in infarct growth and cerebral edema mediated a significant proportion, ~80% of the successful reperfusion effect on functional outcomes.
Future studies on other mediators can help better understand stroke management and identify new therapeutic targets for successful reperfusion effects.
The RapidAI Clinical Affairs team works closely with physicians and healthcare systems worldwide to advance stroke care. Learn more about how we support clinical trials here.
Co-authors of this study: Deep K Pujara MBBS MPH MS, Leonid Churilov Ph.D., Clark Sitton MD, Felix Ng MD, Ameer E Hassan DO, Michael G Abraham MD, Spiros L Blackburn MD, Gagan Sharma MS, Nawaf Yassi Ph.D., Timothy Kleinig h.D., Darshan Shah MBBS, Teddy Y Wu Ph.D., Wondwossen G Tekle MD, Ronald F. Budzik MD, William J Hicks II MD, Nirav Vora MD, Randall C Edgell MD, Diogo Haussen MD, Santiago Ortega Gutierrez MD, Gabor Toth MD, Laith Maali MD, Mohammad Ammar Abdulrazzak MD, Faisal Al-Shaibi MD, Tareq AlMaghrabi MD, Vignan Yogendrakumar MD, Faris Shaker MBChB, Osman Mir MD, Ashish Arora MD, Kelsey Duncan MD, Sophia Sundararajan MD Ph.D., Amanda Opaskar MD, Yin Hu MD, Abhishek Ray MD, Jeffrey Sunshine MD, Nicholas Bambakidis MD, Sheryl Martin-Schild MD, M. Shazam Hussain MD, Raul Nogueira MD, Anthony Furlan MD, Cathy A. Sila MD MS1, James C Grotta MD, Mark Parsons BMed Ph.D., Peter J Mitchell MMed, Geoffrey A Donnan MD, Stephen M Davis MD, Gregory W Albers MD and Bruce CV Campbell MBBS PhD3 on behalf of the SELECT, EXTEND-IA, EXTEND-IA TNK, and EXTEND-IA TNK Part-II Investigators.