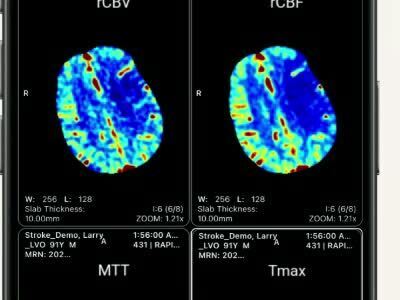
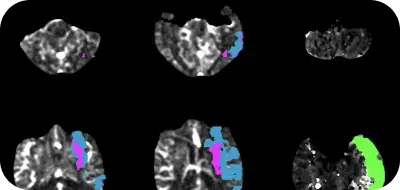
Approximately 240,000 people in the United States experience a transient ischemic attack (TIA) annually. A TIA is a stroke lasting only a few minutes when the blood supply to part of the brain is briefly interrupted.
The risk factors for a transient ischemic attack include:
- high blood pressure
- medical history of heart disease
- diabetes
- blood clots
- atrial fibrillation
- other risk factors like smoking and alcohol abuse
TIAs are associated with an increased risk of debilitating recurrent stroke. Prompt diagnosis at the onset of stroke symptoms and identification of modifiable risk factors can help guide treatment to prevent recurrent strokes.
Complete neurovascular imaging of patients with suspected TIA can help prevent future strokes.
Neuroimaging helps to establish a TIA diagnosis and identify high-risk lesions in the cervical and intracranial arteries that could increase the chances of subsequent stroke.
The multidisciplinary society guidelines recommend performing prompt neuroimaging in patients who present with TIA, preferably within 48 hours of symptom onset.
However, an analysis of Medicare data found that 70.1% of TIA patients discharged from the emergency department with an incomplete imaging workup did not complete the imaging workup as an outpatient.
In a recent study, Dr. Vincent M. Timpone and co-authors obtained Medicare data of 111,417 TIA patients admitted to the emergency department at 4,253 unique hospitals and found incomplete neurovascular imaging was associated with higher odds of subsequent stroke within 90 days (OR 1.3 [95% CI: 1.23-1.38]).
Detecting ischemic lesions in TIA patients
Confirming TIA diagnosis can be challenging since the clinical deficits resolve by the time of evaluation as this type of stroke lasts only a few minutes before symptoms disappear.
While TIA diagnosis can help initiate preventive treatment and avert the risk of a subsequent debilitating ischemic stroke, it can also help identify TIA 'mimics' and avoid inappropriate treatment.
Several studies have confirmed the sensitivity of diffusion-weighted imaging (DWI) analysis in detecting ischemic lesions in TIA cases. The rate of positive DWI in these studies varied from 16% to 67% among suspected TIA cases.
Dr. Mlynash and co-authors, in a prospective study, found that a combination of early DWI and perfusion-weighted imaging (PWI) could document the presence of cerebral ischemic lesions in approximately half of all patients with suspected hemispheric TIA.
DWI can help establish the ischemic etiology in patients with TIA symptoms. With higher sensitivity, PWI can help confirm DWI results and reveal hypoperfusion in patients with a negative DWI.
Increasing access to advanced neurovascular imaging for TIA patients could facilitate early detection and treatment of modifiable risk factors for subsequent stroke.
Artificial intelligence tools like RapidAI can support ED physicians and accelerate clinical decision-making. RapidAI is the only platform that provides both CT and MR perfusion solutions.