Venous thromboembolism (VTE) can be as challenging to diagnose as it is to treat, and research shows that very few patients have a strong understanding of the condition and its symptoms, often preventing many from seeking care until it is urgent — if at all. Fortunately, new models are being developed to effectively capture more VTE patients before it becomes too late.
One interdisciplinary care model is Pulmonary Embolism Response Teams, or PERTs. They are designed to help physicians better manage PE, improve care coordination, and determine the best treatment for acute PE patients. In fact, research has shown that PERT team evaluation for patients reduces that patient’s mortality at 30-90 days, even for patients who don't receive any additional intervention.
When we think about what PE care looks like in the future, it is impossible to not speak about the advanced tools leveraging the power of AI to help us streamline care, boost team efficiency, and improve acute PE patient outcomes. Despite the promise that PERTs have shown in streamlining patient care, advanced technology is also showing great potential in filling in the remaining gaps.
Dr. Jimmy Kerrigan, Interventional Cardiologist, and his team at Ascension Saint Thomas Heart implemented this practice earlier this year to support a more proactive — and ultimately more effective — approach to PE care. He shares three impacts of AI that can further support PERTs.
Timely Detection and Risk Stratification
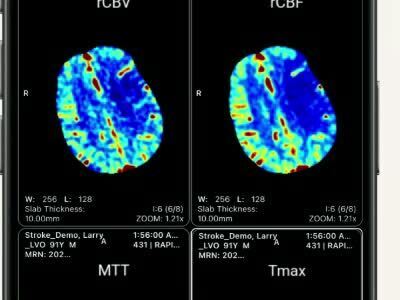
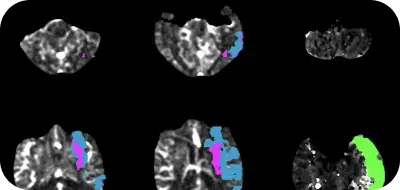
AI can improve the identification of PE patients and enable physicians to prioritize their efforts. By automatically analyzing CTPA images, identifying suspected pulmonary embolism, and delivering real-time notifications to physicians, patients can be triaged faster and care teams aligned more quickly, reducing overall time to treatment.
Optimizing Workflow and Communication
Even with a formalized PERT program, PE care can sometimes be a disjointed process. For example, when PERT is activated, physicians may get a page or phone call, find a computer to log into the EMR or PACS to review the CT, labs, and vitals, and then have to log into another HIPAA-compliant texting app to communicate with the rest of the care team. Platforms like RapidAI are one example of leveraging advanced technology to further streamline and operationalize this multi-step process, better connecting physicians through one easy-to-use platform for clinical data updates, image previewing and communication.
Connecting the loop of patient care and integration into the EMR
Research shows that of those who experience and survive a PE, one-third will have a recurrence within 10 years. Integrating workflow apps with the EMR can not only play an important role in giving responding physicians more information about a patient’s clinical status in determining treatment path, but also by improving the opportunities to ensure appropriate patient follow-up after discharge.
As PERT programs continue to increase in popularity, and AI-enabled technologies continue to become more capable and more widely available, the two combined hold enormous potential for not only complementing, supporting, and enhancing physician processes but also truly optimizing VTE care and improving patient outcomes.
To learn more about the next evolution of VTE care, check out Dr. Kerrigan’s full article in Vein Magazine.