It is well known that endovascular thrombectomy (EVT) improves clinical outcomes in ischemic stroke patients with an LVO in the anterior circulation.
However, does the choice of anesthesia during the thrombectomy procedure affect outcomes?
Dr. Amrou Sarraj and co-authors hypothesized that general anesthesia (GA) might be associated with worse clinical outcomes following EVT than non-GA, especially in patients with worse collaterals. They performed a pooled patient-level analysis to test this hypothesis.
Key takeaways:
- General anesthesia was independently associated with worse functional outcomes after EVT (p=0.021), and the association was sustained in a model adjusted for hypoperfusion intensity ratio (p=0.019).
- General anesthesia was also associated with higher rates of neurological worsening (p=0.045) and numerically higher mortality (p=0.06).
Study design
Patients from three randomized clinical trials, EXTEND-IA, EXTEND-IA TNK, and EXTEND-IA TNK part II, along with patients from SELECT, a prospective cohort study, were pooled for this study. All patients in these trials were treated with EVT for anterior circulation LVO.
The patients were stratified based on the type of anesthesia, GA vs. non-GA. Non-GA patients received conscious sedation or local anesthesia without sedation.
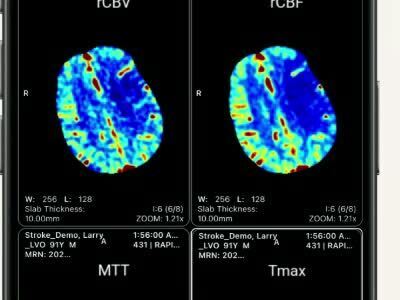
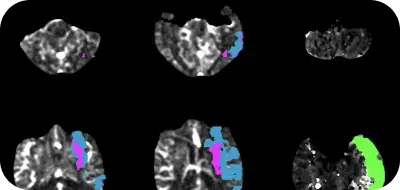
All patients received non-contrast CT (NCCT), CT angiogram, and CT perfusion before EVT. The collateral status was determined using Rapid CTP based on the automated hypoperfusion intensity ratio.
A hypoperfusion intensity ratio (HIR)<0.4 was considered good collaterals, and an HIR≥0.4 on perfusion imaging was considered poor collaterals.
The distribution of the 90-day mRS score was the primary outcome. The secondary outcome was functional independence (mRS 0-2) at 90-day follow-up.
Functional outcomes and anesthesia type
Of 725 patients treated with EVT, 299(41%) received GA, and 426(59%) non-GA. However, the baseline characteristics between patients who received GA and non-GA were significantly different. Therefore, 182 matched pairs of patients receiving GA vs. non-GA were identified using propensity scores.
After adjusting for confounders, GA was found to be independently associated with worse functional outcomes (p=0.021). The association was sustained in a model adjusted for HIR (p=0.019).
Furthermore, GA was associated with higher rates of neurological worsening (GA: 14.9% vs. non-GA: 8.9%, p=0.045) and numerically higher mortality (GA: 14.3% vs. non-GA: 8.8%, p=0.06).
Collaterals and anesthesia type
With good collaterals, no differences were observed in the distribution of mRS scores at the 90-day follow-up between patients who received GA and non-GA. However, in patients demonstrating poor collaterals on perfusion (HIR≥0.4), GA was associated with worse functional outcomes (p=0.002) compared to patients who received non-GA. The interaction of thrombectomy outcomes by anesthesia type was approaching but not reaching statistical significance (Pinteraction = 0.07).
With poor collaterals, neurological worsening (GA: 19.3% vs. 8.6%, p=0.018) was significantly higher, and mortality (GA: 18.3% vs. non-GA: 12.1%, p=0.078) was numerically higher with GA.
No difference was observed in infarct growth in patients with good collaterals. In contrast, patients with poor collaterals demonstrated a larger infarct growth with GA (p=0.022). Notably, there was a significant interaction between collaterals and anesthesia type on infarct growth rate (Pinteraction=0.020).
This study provides Class III evidence that GA is associated with worse functional outcomes in patients undergoing EVT.
RapidAI has been used in some of the most influential stroke clinical trials, producing high-quality data to redefine stroke care. The RapidAI Clinical Affairs team works closely with physicians and healthcare systems around the world to advance stroke care. Learn more how we support clinical trials here.