In 2022, the RapidAI clinical affairs team partnered with physicians across therapeutic areas to help advance research and improve patient outcomes.
Here’s a look at some of the publications from this year by physicians using RapidAI, showing us how the software is making a difference in patient care.
Aneurysm
Supporting aneurysm detection and management.
AI-enabled measurement tool Rapid Aneurysm identified growth in volume, surface area, and maximum size of aneurysms
Dr. Daniel Sahlein and co-authors performed a retrospective study to determine whether the reproducible volumetric and surface area measurements of aneurysms by Rapid Aneurysm can accurately reflect aneurysm size and hence aneurysm growth over time.
The results showed that Rapid Aneurysm had a higher sensitivity for detecting changes in aneurysm size than the current clinical practice, which uses manual linear measurement. Rapid Aneurysm was able to identify growth in aneurysm volume, surface area, and maximum size. Multiple aneurysm experts have indicated that these study results will have a profound impact on the future of aneurysm management.
Rapid Aneurysm had high sensitivity and specificity
Dr. Jeremy Heit and co-authors performed a retrospective cohort study to investigate the accuracy of Rapid Aneurysm in detecting unruptured cerebral aneurysms on CT angiography (CTA).
Four expert neuroradiologists screened the CTA scans and helped set the reference standard. The expert neuroradiologists detected 60 aneurysms, and Rapid Aneurysm detected 57 aneurysms. Rapid Aneurysm had 95% sensitivity, 100% specificity, and 99.7% accuracy. The positive predictive value was 100%, and the negative predictive value was 99.7%.
Stroke
Helping optimize patient selection for advanced treatment.
Perfusion Imaging Predicts Favorable Outcomes after Basilar Artery ThrombectomyA multicenter collaboration of Rapid users developed a scale to predict which patients are most likely to benefit from thrombectomy for basilar artery occlusion (BAO). The investigators created a Critical Area Perfusion Score (CAPS), which quantifies severe hypoperfusion (Tmax > 10) in the cerebellum pons, and midbrain/thalamus. Patients with a low CAPS had a favorable response to reperfusion following thrombectomy. However, patients with more extensive regions of hypoperfusion in critical brain regions (high CAPS) did not benefit from endovascular reperfusion. These pilot date led to an NIH-funded study called PRECISE which is a large prospective study that aims to validate these findings.
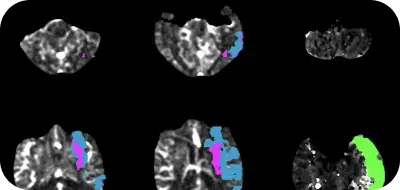
Assessing perfusion mismatch volume using Rapid software in childhood arterial ischemic stroke patients.Treating children with arterial ischemic stroke (AIS) is challenging due to delayed diagnosis and the inability to determine the safety and efficacy of advanced treatment options. Melissa J. Vissers and co-authors conducted a retrospective study to explore the feasibility of Rapid MRI to determine the mismatch characteristics in childhood AIS patients. The study showed that Rapid MRI could assess diffusion/perfusion mismatch volumes, and potentially identify salvageable tissue, in childhood AIS patients.
Using Rapid CTP to predict final infarct volume in basilar artery occlusion patientsThe optimal CTP parameters to select basilar artery occlusion (BAO) patients for EVT are unknown. Dr. Nicole Yuen and co-authors performed a retrospective study (using Rapid CTP) to determine the CTP parameters that best predicted the final infarct volume in BAO patients who were successfully revascularized after EVT.
Several time-to-maximum (Tmax) and cerebral blood flow (CBF) thresholds were used on the pre-EVT CTP scans to determine the best predictor of the final infarct volume.
Tmax >8s (R2, 0.56; median absolute error, 16.0 mL) and Tmax >10s (R2, 0.73; median absolute error, 11.3 mL) were the strongest predictors of the post-EVT final infarct volume. CBF <38% (R2, 0.76; median absolute error, 8.2) and CBF <34% (R2, 0.76; median absolute error, 9.1 mL) also performed well for final infarct estimation and correlated well with final infarct volume on DWI.
Supporting stroke research that will improve understanding of stroke pathophysiology and patient care.
Accuracy of CT Perfusion-Based Core Estimation of Follow-up Infarction
There has been uncertainty regarding the accuracy of CT Perfusion-based ischemic core estimation for patients who are imaged early after symptom onset. In this substudy of the SELECT trial, overestimation of irreversibly injured ischemic core volume was rare using Rapid CTP, and limited to patients scanned within 90 minutes of last know well time. Using a rCBF threshold of <20% for these early arriving patients eliminated overestimation.
Biomarkers to predict intracranial atherosclerotic stenosis-related LVO
Intracranial atherosclerotic stenosis (ICAS) is one of the leading causes of large vessel occlusion (LVO). However, it is challenging to diagnose ICAS-related LVO. Can hypoperfusion intensity ratio and cerebral blood volume index help diagnose underlying ICAS?
Dr. Yukihiro Imaoka and co-authors hypothesized that lower HIR and higher CBV index would be helpful biomarkers to predict underlying ICAS before EVT. In a retrospective study with 43 patients, Rapid CTP was used to analyze their CTP images. Results suggested that an HIR ≤ 0.22 and a CBV index ≥ 0.9 could help predict ICAS.
Anesthesia choice for EVTDoes the choice of anesthesia during the thrombectomy procedure affect outcomes? Dr. Amrou Sarraj and co-authors hypothesized that general anesthesia (GA) might be associated with worse clinical outcomes following EVT than non-GA, especially in patients with worse collaterals.
They performed a pooled patient-level analysis and found that GA was independently associated with worse functional outcomes after EVT in patients with poor collateral but not among patients with favorable collaterals. Rapid CTP’s automated hypoperfusion intensity ratio was used to determine collateral status.
tPA administration and venous outflow profileCan early tPA administration in acute ischemic stroke patients improve the venous outflow (VO) profile in the baseline CTA performed before EVT? A good VO profile is associated with a higher likelihood of reperfusion following EVT.
In the retrospective cohort study, Dr. Tobias Faizy and co-authors found that administering tPA before EVT in LVO patients was independently associated with favorable VO profiles on baseline CTA imaging. Patients who received tPA before EVT also had more favorable functional outcomes 90 days after treatment. The CTP scans were processed using Rapid CTP to determine the core and penumbra volumes.
A comprehensive cerebral collateral cascade analysis in ischemic stroke patientsCan a comprehensive cerebral collateral cascade (CCC) analysis help predict clinical and radiological outcomes in patients treated with EVT? In a retrospective, multicenter cohort study, Dr. Tobias Faizy, and co-authors used multiparametric CT imaging to assess the CCC of LVO patients that underwent EVT.
The study results showed that a comprehensive assessment of the collateral blood flow cascade could help predict the clinical outcomes of thrombectomy treatment in LVO patients. A favorable CCC profile indicates good functional results in LVO patients undergoing thrombectomy. Patients with favorable CCC profiles had considerably lower final infarct volumes. Rapid CTP was used to analyze all the CTP images.
Sex differences in WAKE-UP stroke trialSex-based differences have been reported in stroke settings. Women often present with more severe stroke symptoms. Dr. Anke Wouters and co-authors performed a post-hoc analysis of the WAKE-UP trial data to explore the sex-based differences in baseline imaging, clinical characteristics, and outcomes.
In the WAKE-UP trial, women were older (p<0.01), had higher baseline NIHSS (p<0.01) and mRS (p=0.04) and smoked less frequently. They also presented with more aphasia than men (p = 0.01). Imaging characteristics did not differ between the sexes, and there was no effect of sex on the clinical outcome after treatment with alteplase. Rapid software calculated the ischemic core, volume, and hypoperfusion intensity ratio.
We look forward to continuing our support of clinical research and collaborating with physicians worldwide. Subscribe to the RapidAI blog to learn about our latest work and publications.