An analysis of large vessel occlusion (LVO) patient data collected before and after the stroke team’s adoption of the Rapid Workflow for Stroke mobile app at Johns Hopkins University School of Medicine showed a significant reduction in intrahospital treatment times.
The findings of Dr. Mais Al-Kawaz and co-authors were published in the Journal of Neurointerventional Surgery.
Key takeaways:
- There was significant reduction in door to groin puncture time (DGPT), door to first pass time (DTFP), and door to recanalization time (DRT) following the installation of the Rapid Workflow for Stroke mobile app at Johns Hopkins University School of Medicine (a comprehensive stroke center)
- The Rapid Workflow for Stroke mobile app can result in a significant reduction in stroke care delays, ultimately improving neurologic outcomes following clot removal.
With studies showing that reducing door to groin puncture time and door to recanalization time can improve a patient’s neurological outcome, stroke teams are adopting AI solutions to provide clinical decision support and help optimize stroke workflows to reduce time to treatment.
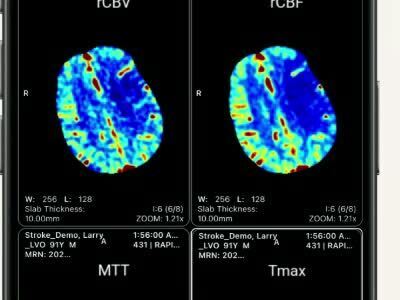
The purpose of this study was to understand the impact of the Rapid clinical platform and mobile app on intrahospital treatment times and stroke workflow. The Rapid Workflow for Stroke mobile app aids stroke teams by quickly notifying them when new patient data is available and providing them easy access to preview advanced Rapid results and source images directly from their mobile device.
Data from 64 patients who presented with an LVO was included in this study.
31 patients were admitted between June 2019 and March 2020, before the installation of the Rapid Workflow for Stroke mobile app. 33 patients were admitted between March 2020 and October 2020, after installation of the Rapid Workflow for Stroke mobile app.
The average age, risk factors, and the presenting National Institutes of Health Stroke Scale (NIHSS) of the two groups were comparable. Most patients in both groups were diagnosed with proximal M1 occlusions.
The Rapid Workflow for Stroke mobile app helped reduce door to groin puncture time by 33 minutes
The mean treatment times before and after the installation of Rapid Workflow for Stroke mobile app were compared.
- 33 minutes saved: DGPT decreased significantly from 104±9 minutes to 71.1±51.7 minutes (p = 0.02).
- 35 minutes saved: DTFP time decreased significantly from 131.9±8 minutes to 97.2±55.9 minutes (p=0.02).
- 37 minutes saved: DRT decreased significantly from 148.1±1 minutes to 110.7±56.6 minutes.
This study did not include Rapid in-app communications for team activation and alignment on patient care which has been found to further improve time savings.
Following the installation of the Rapid Workflow for Stroke mobile app, patients had a significantly lower NIHSS at 24 hours post surgery and at discharge.
The mRS values at 3 months post surgery were comparable between the two groups. However, data was only available for 29 patients in the pre-app group and for 24 patients in the post-app group and hence difficult to interpret.
The Rapid Workflow for Stroke mobile app can help stroke teams improve treatment times through the notification of results availability, previewing of Rapid results and source images from anywhere, anytime.
Save time with immediately available post-treatment case summary
Rapid Workflow for Stroke mobile app users who have activated its communications functionality, can now access immediate case summaries, and send them to their email at the push of a button
Case summaries provide a comprehensive snapshot of the patient’s journey and includes all the information that has been entered into the app, from prehospital routing to triage, activity time stamps, communication and workflow data, Rapid results, and outcomes. Administrators can review the case summaries and workflow metrics and use the data to deliver better patient care.
Check out how you can streamline stroke care coordination using RapidAI.