In today’s climate with COVID-19 continuing to drain hospital resources worldwide, the time care teams spend on making clinical decisions is more valuable than ever. More and more hospitals are turning to tools that leverage the power of artificial intelligence (AI) to help streamline care, boost team efficiency, and improve patient outcomes. AI can help extract greater meaning and insight from a patient’s medical information that ultimately helps physicians improve patient care. These solutions are often paired with patient workflow and communication apps for easier care coordination and efficient team communication. Given the time- and resource-intense needs of diagnosing, risk-stratifying, and treating pulmonary embolism (PE) patients, AI-assisted solutions warrant consideration.
A difficult diagnosisQuick and accurate risk stratification is key, not only for the benefit of the patient but for the efficient use of strained hospital resources. But PE patients are a particular challenge: there is no single non-invasive test that is both sensitive and specific to PE. Symptoms of PE varies dramatically, from patients being asymptomatic to those with complete cardiovascular collapse. Further, PE symptoms can be vague or non-existent, and the clinical presentation shares features with many other common diagnoses.
Even at sites of care with standardized protocol for PE, quickly aligning on an accurate diagnosis requires sharing results of multiple tests and imaging files with a number of specialists. In many settings, this means multiple phone calls, text alerts, voice mails, playing phone tag, repeating information, and more.
A particularly resource-demanding PE patient subgroup: intermediate high risk
Once a patient is risk stratified, treatment plans are complex and individualized requiring clear communication among team members. This is especially true for those intermediate-high risk stratified patients characterized by positive simplified Pulmonary Embolism Severity Index (sPESI), right ventricular (RV) dysfunction, and elevated troponin. Studies have shown that normotensive patients with both RV dysfunction and elevated troponin are at a higher risk of short-term death. As such, close monitoring of these patients is required so that treatment plans can be quickly adjusted if necessary.
The optimal management of the intermediate-high risk group remains to be defined. Given a wide range of possible treatment options is available, multidisciplinary discussion of those options – and the risks and benefits of each – is required. Gathering the specialists and easily disseminating patient information remains a challenge.
How AI-powered and assisted solutions can help streamline care and improve team efficiency
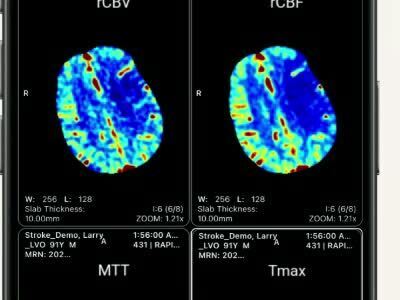
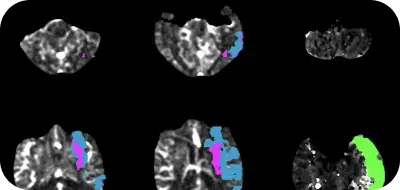
AI-powered and assisted solutions can help reduce the burden on hospital staff when managing PE patients. New AI tools can help to rapidly identify suspected pulmonary embolisms by automatically processing CTA scans. This information can be quickly and automatically distributed to PE team members’ mobile phones or laptops, helping physicians speed risk stratification and prioritization of PE patients.
Clinical decision support tools become even more powerful when combined with patient workflow and care team coordination apps. These apps provide an efficient way to organize patient history and share imaging/ test results. Centralizing this information, accessible from a smart phone or laptop, means everyone is working from a single, up-to-date view of the patient.
For high-resource consuming patient groups like intermediate-high risk PE patients, the ability to quickly connect multiple specialists to align on a course of treatment means more efficient use of stretched resources. These care coordination apps facilitate virtual meetings where the various treatment options can be discussed in real time and a course of treatment quickly decided upon. HIPAA-compliant messaging provides an easily accessed history of conversations. No more phone tag, voicemails, and precious time spent coordinating critical consultations.