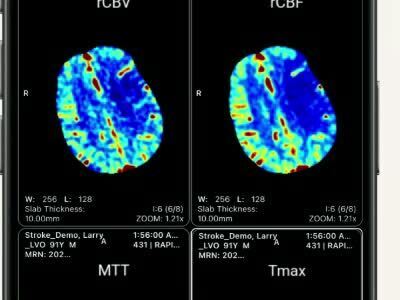
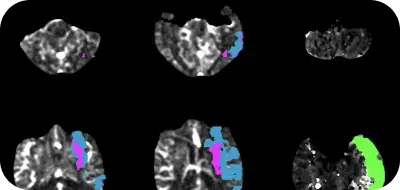
In the last two decades, we have seen tremendous advances in cerebrovascular neurosurgery, with new noninvasive imaging techniques, medical devices and treatment options. Randomized clinical trials (RCTs) provided evidence on the safety and efficacy of these new interventions.
However, RCT populations are not always representative of the broader patient population encountered in clinical practice. Factors like time constraints, lack of resources, costs, and regulatory requirements, often lead to narrow and strict inclusion criteria in RCTs.
By collecting real-world clinical data from a broad spectrum of patient populations, the Stroke Thrombectomy and Aneurysm Registry (STAR) helps optimize patient selection for new treatment interventions outside of RCT criteria.
We spoke with Dr. Alejandro Spiotta and Dr. Ali Alawieh, the founders of STAR, to learn more about the registry and its impact on acute stroke management.

Dr. Alejandro Spiotta

Dr. Ali Alawieh
1. What led you, Dr. Spiotta and Dr. Alawieh, to start the registry? How did the idea come about?
When thrombectomy became the standard of care for a select population of stroke patients, we quickly realized that the effect size of this intervention is one of the largest treatment effects in medicine. This eventually led to the expansion of indications for thrombectomy to include patient populations/devices/techniques that were not included in the original trials.
There was a need to obtain high quality real-world data to determine the efficacy and safety of these interventions in patients who did not meet the original trial criteria and across patient subpopulations. Such analyses required collaboration across different centers at a large scale to yield generalizable and robust results. We started the registry with this goal.
When we contacted some of our collaborators in the U.S., there was great enthusiasm for this project. Within the first few months, we published 5 papers and enrolled 7 centers. Soon, we started seeing interest from more stroke centers in the U.S. and across the globe.
2. What is the mission of STAR?The mission of STAR is two-fold:
- Improve outcomes of patients suffering from ischemic and hemorrhagic stroke via real-world, high-volume, high-quality clinical research
- Foster international collaboration and create a network to advance stroke management through research and shared experiences.
3. In your opinion, what has been the biggest impact STAR has had on stroke management thus far?
STAR provided us with insights into the significance of procedure time on thrombectomy outcomes indicating that returns can be diminished following 3-attempt or 60-minute cut-off.
STAR was the first to show, using high-volume data, that treatment efficacy is maintained in patients with posterior circulation stroke and is comparable to treatment efficacy in patients with anterior circulation stroke. It also showed that the stent retriever technique has a higher rate of hemorrhage compared to aspiration, supporting the use of the latter approach in this patient population.
We published a series of papers and identified the optimal blood pressure management protocol for patients undergoing thrombectomy.
Data from STAR provided pivotal insights during the COVID-19 pandemic revealing how the pandemic led to workforce depletion in Neurointerventional Units. The pandemic also affected stroke outcomes and patient demographics.
4. Why is it important to include global data to the registry?
One of the aims of STAR is to support physicians across health systems to deliver high-quality care for patients with stroke. Gathering data from across the world and from different health systems is critical to this effort.
5. How can new sites join STAR?
New sites can join STAR by:
- Emailing STAR directly or
- Submitting a request to join application via our online portal -https://redcap.musc.edu/surveys/?s=HE9X3XHNJL
Once the STAR team receives the request, our team will correspond with the site to assist with IRB approval and data use agreement. After we get all the approvals, we will provide a secure online portal link to help transfer data. Our team will also continuously monitor the incoming data for accuracy and share feedback.
Follow STAR’s website to learn more about the network and research and to take part in their discussions.
Check out "Why RapidAI for Stroke" and learn how our advanced imaging technology is optimizing patient selection for thrombectomy.