Although 98% of healthcare leaders say their organization is implementing an AI strategy, adoption within the emergency room has remained somewhat limited until recently.
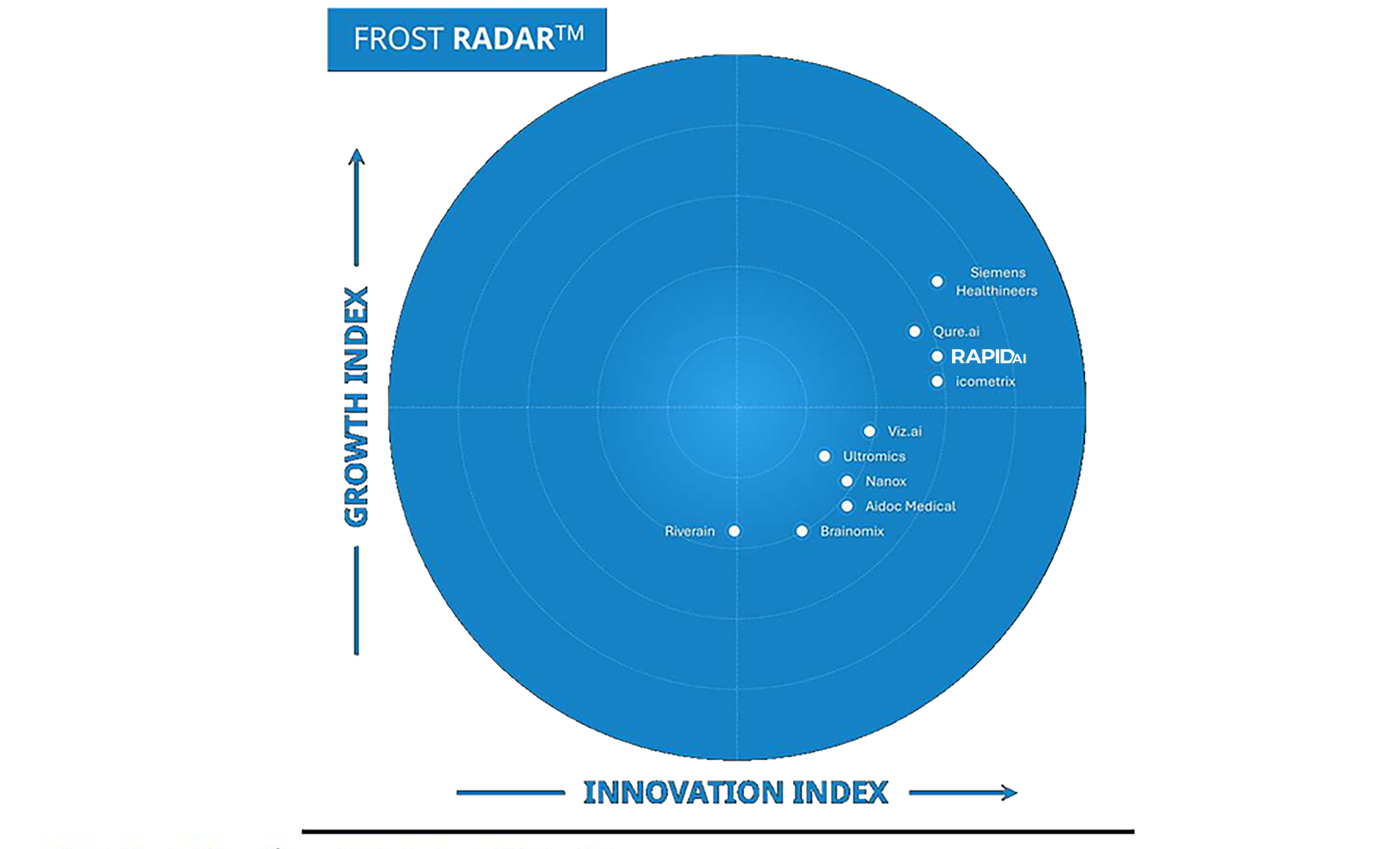
COVID-19 shed new light on the inefficiencies that have long plagued emergency care and as AI-powered technologies like RapidAI continue to demonstrate their clinical, operational, and financial value, a growing number of hospitals are exploring new technologies aimed at improving diagnosis, communication, workflow, and ultimately patient outcomes.
One reason hospitals are keen to implement innovative technology is the promise they offer to improve care. Research has found that for every 10-minute delay between arrival at the emergency room (ER) and starting stroke treatment, patients with severe strokes may lose eight weeks of “healthy life.”
Rachel Witalec, VP of Product and Strategy at RapidAI, shares six considerations for vetting and implementing AI technologies, including:
1. Modernize Thoughtfully. Technology doesn’t need to be complex to be valuable. Evaluate technology for both promise, but also sensibility. For example, new tools should unquestionably alleviate physician burnout, rather than contribute to it.
2. When In Doubt, Lean into Clinical. The best technologies will likely attract the best minds, so consider the medical experts involved in the product’s development, look to key opinion leaders you trust, and expect clinical validation throughout the process.
3. Think End-to-End. Look for technologies that show it connects teams, rather than keeps them in silos. The reality of acute care is that connection is absolutely critical from the beginning, so that all teams are aligned to drive the best patient outcomes.
4. Keep Interoperability & Transparency Top of Mind. Interoperability is crucial for solutions to integrate with your current technologies and processes, but also those you may consider down the road. Along with this, transparency better positions healthcare systems in the long run by identifying gaps in privacy, biases, and accuracy — ultimately supporting equitable and ethical patient care.
5. Bring Key Stakeholders into the Process. Physicians, nurses, and participating support staff should have the loudest say in whether the new technology is the right fit or not.
6. Demand Data to Measure Impact. Choose tools that give you strong and plentiful data on usage, efficiency, and outcomes to ensure you know how it’s working, yielding ROI, and identifying where your team and technology can improve.
To learn more about assessing the right technology for your organization, check out Rachel’s full article in Healthcare Business Today here: Identifying the Right Technology to Streamline Your Hospital Workflow.